What is a Retinal Detachment?
Retinal detachment is a serious eye condition that requires urgent assessment and emergency surgery. A detached retina occurs when the retinal lining detaches from the back of the eye. It is often compared to to wallpaper peeling off a wall, where the wall paper represents the retina, the light-sensitive layer at the back of the eye. When the retina is detached and separated from the inner surface of the eye, vision can be threatened and it may lead to permanent vision loss if left untreated. This means urgent assessment and timely access to surgery is absolutely crucial in retinal detachment treatment.
What Causes a Retinal Detachment?
Approximately one in 10,000 people suffers from a retinal detachment. Retinal detachment can occur due to a retinal tear or a break in the retina. The fluid from the vitreous jelly seep under the retinal lining causing the retina to lift off. Retinal detachment may occur due to previous eye trauma or complications from previous eye surgery. Being short-sighted (myopia) increases the risk of developing a detached retina. In some cases, there may be a family history of retinal detachment.
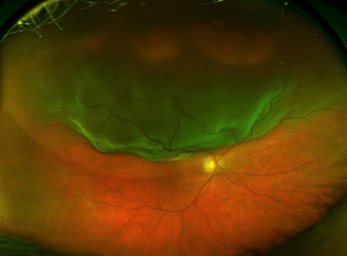
What are the Symptoms of a Retinal Detachment?
Symptoms of a retinal detachment you may notice include:
- Sudden onset of flashes of light
- Sudden onset of floaters – dark spots or blobs, a shower of black sooty dots, ‘cob-web’ like floaters
- Sudden loss of vision
- An impression that there is a curtain moving up and down or sideways
- Vision on one side of the field may be reduced or blurred
- In addition to the blurred vision, you may notice a reddish or pinkish tinge to your vision
- You may not notice a vision change or have any symptoms but the detached retina can be detected during a routine eye examination. This depends on the location of the retinal detachment
What is the Treatment for a Detached Retina?
Treatment for retinal detachment involves surgical repair with vitrectomy surgery and/or scleral buckle, gas, silicon oil or heavy liquid.
Vitreoretinal surgeons such as Dr Lawrence Lee surgically repair a retinal detachment with vitrectomy surgery. Vitrectomy involves removing the vitreous jelly of the eye. During vitrectomy surgery, Dr Lee uses laser to seal the retina and injects diluted gas (C3F8), silicone oil or heavy liquid to flatten the retina and hold it in place. Diluted gas is usually absorbed over a period of six to eight weeks. Alternatively, silicone oil or heavy liquid is used as a tamponade agent and they are removed at a later stage once the retina heals.
In some cases, Dr Lee would use a scleral buckle in conjunction with a vitrectomy surgery. It is reserved for smaller retinal detachments or dialysis type of detachments. A scleral buckle is a reinforcing silicone band which is placed on the outer wall of the eye to help seal the retinal tear or detachment. It remains in place permanently and becomes part of the eye wall.
What is the Success Rate of Retinal Detachment Surgery?
The success rate for retinal detachment surgery is approximately 90%. Approximately 10% of cases may require further surgery if the retina does not remain attached after the first procedure. Once the retina remains attached for 3 months following the surgery, the incidence of further re-detachment is much less.
Cataract surgery may be required in combination with the vitrectomy repair, or a later time once the retina is repaired.
Following vitrectomy surgery to repair the retina, some patients regain their vision fully. Some may have reduced vision despite the surgery being successful. The improvement in vision depends on whether the macula, the central area of the retina was affected by the detachment. Duration of a retinal detachment prior to getting to the surgery plays a crucial role too. Access to prompt management of a detached retina in a timely manner is important.
How to Choose the Right Surgeon?
Dr Lee’s skills and expertise in emergency retinal detachment repairs have saved the sight of many patients. We make every effort to provide emergency care and triage, urgent admission to the hospital and collaborate with the ophthalmic operating theatre team and anesthetists to ensure the best outcome.
