POLYPOIDAL CHOROIDAL VASCULOPATHY
Polypoidal choroidal vasculopathy (PCV) is a retinal condition characterized by abnormal blood vessels in the choroid. The choroid is a layer of tissue underneath the retina. The abnormal vascular layer of the choroid results in damage to the overlying retina. Here, the photoreceptors act as light-sensing cells responsible for our vision.
PCV is often considered to be similar to age-related macular degeneration. It is more common in people over the age of 60. It is also more common in people with Asian descent.
What are the Symptoms of PCV?
Patients diagnosed with PCV experience similar symptoms to macular degeneration such as blurred or distorted vision. They may also have a grey patch (scotoma) near the centre of vision. The onset of symptoms may occur over weeks to months. In some cases, however, symptoms can occur suddenly. Your retinal specialist may even diagnose PCV before it has caused any symptoms. Although PCV appears to affect only one eye in some patients, it can go on to affect both eyes over time. So, frequent monitoring is important.
How is PCV Diagnosed?
The most important test is a comprehensive eye examination by your retinal specialist. Diagnostic testing involving the use of fluorescein angiography and indocyanine green (ICG) angiography is particularly useful. Detailed photographs of the blood vessels in the retina and underlying choroid are taken. This helps your retinal specialist in identifying important abnormal blood vessels. The abnormal vessels typically appear “balloon-like” or they may look like “polyps”. These abnormal blood vessels in PCV can leak fluid or blood into and under the retina. This causes vision loss and scarring of the retinal tissue over time. Loss of vision can be sudden if the abnormal blood vessel bleeds and results in a large haemorrhage in the eye.
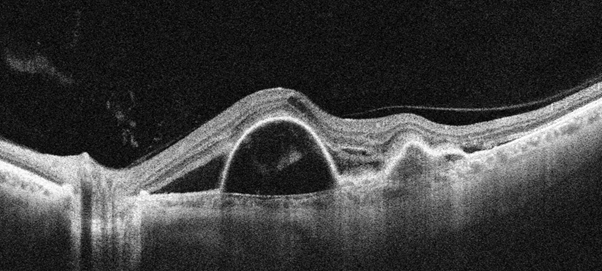
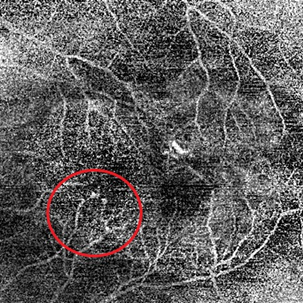
Optical coherence tomography (OCT) scanning and OCT angiography (OCT-A) are also very useful. They assist in the diagnosis of PCV, monitoring the condition, and assessing how the patient responds to treatment.
What are the Treatment Options and Prognosis of PCV?
Current treatments for PCV involve intravitreal injections of an anti-VEGF medication (eg. Eylea or Eylea HD), photodynamic therapy (PDT), or a combination of both.
Vascular endothelial growth factor (VEGF) is a molecule generated by the body. It causes the abnormal vessels to leak fluid or bleed. Injections of anti-VEGF injections block the activity of VEGF. As a result, there is a decrease in the leakage of fluid or blood from the abnormal vessels. Successful management of PCV often requires regular anti-VEGF treatment. In some cases, photodynamic therapy (PDT) may be required in combination with the anti-VEGF therapy. This further optimizes the treatment option as the PDT laser is applied to destroy the abnormal blood vessels in PCV. On rare occasions, vitrectomy surgery may be required if a patient has suffered a large bleed or haemorrhage caused by PCV.
Unfortunately, some patients with PCV may experience irreversible vision loss in one or both eyes. Early diagnosis is therefore very important. Prompt treatment may restore vision in some patients and regular monitoring is vital in preventing further vision loss.
Do you have questions or concerns about your eye health or a specific eye condition? To discuss, please contact City Eye Centre for more information.patients and regular monitoring is vital in preventing further vision loss.
