Macular degeneration, also known as age-related macular degeneration, AMD or ARMD, is responsible for 50% of legal blindness cases in Australia. It is estimated that one in seven Australians over 50 years of age show signs of macular degeneration. 1.7 million Australians currently live with macular degeneration and a staggering 8.5 million Australians are at risk of developing this sight-threatening condition. These figures are projected to increase due to an ageing population.

There are different stages of macular degeneration based on clinical signs: early, intermediate and late. In the early stage, vision is usually normal and some drusen, pigment changes and clumping are noted at the macula (central part of the retina used for detailed vision such as reading). It is important that you are monitored regularly and an OCT scan is important to monitor for any new changes.
In the intermediate and late stages, leakage and bleeding from the abnormal blood vessels under the retina (called choroidal new vessels) can occur, and they can occur rapidly. This may lead to sudden onset of vision loss or distortion and requires urgent assessment and treatment. This is termed wet or neovascular macular degeneration. There may be variants associated with similar pathology such as myopic retinopathy, polypoidal choroidopathy, and mactel.
Alternatively the retina may become thinned (atrophic) with loss of photoreceptors at the macula leading to scotomata (gaps) in vision. This usually occurs gradually but it can also accelerate, particularly in those who also have advanced macular degeneration in the other eye or a family history of macular degeneration. This is termed late dry macular degeneration.
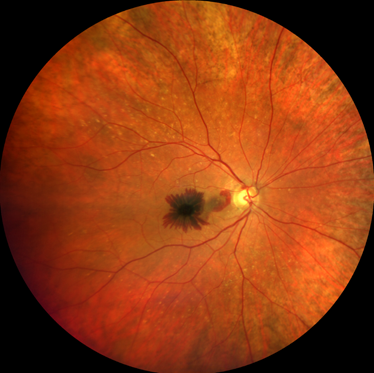
Macular degeneration treatment options with anti-VEGF therapy
Current treatments for Wet (Neovascular) macular degeneration include intravitreal injections with agents such as Eylea (aflibercept), Lucentis (ranibizumab), and Vabysmo (faricimab).
These drugs are anti-vascular endothelial growth factor (anti-VEGF) agents and they act by inhibiting the growth of abnormal blood vessels and help prevent further leakage of these blood vessels. They have been highly effective in preserving vision in the wet form of macular degeneration where there is leakage and bleeding.
Many of our patients have successfully stabilized their vision for many years, through prompt diagnosis, thorough follow-ups and regular intravitreal anti-VEGF injections.
Syfovre (pegcetacoplan) and Izervay (avacincaptad pegol) are new treatments on the horizon for the type of macular degeneration characterized by geographic atrophy (thinning).
What is involved in an intravitreal injection?
Injection of these drugs is performed as an outpatient procedure in our clinic. Topical, local and peribulbar anaesthetic is used and therefore the injection should have minimal pain. Patients who have anxiety can be managed with sedation. After the injection, antibiotic eye drops such as Chlorsig are administered four times a day for three days to help prevent infection.
Some patients may feel irritation on the first day after the injection, as well as tearing and redness in the eye. Topical lubricants such as Systane may be useful.
If you notice any persistent pain, redness or changes in your vision, you should contact City Eye Centre. Generally, complications are very rare but they may include intraocular infection, uveitis, vasculitis, lens damage and retinal detachment and require urgent treatment.
Up to 80% of patients notice improvement after their first injection. Most patients require monthly injections for the first three months and OCT scans to monitor the progression and response to treatment. Following this, the interval between treatments may gradually be extended. Further treat and extend may be possible with some patients stable on 3 monthly treatment intervals of treatment. Treatment will be tailored by your Doctor according to the response to the treatment plan.
Eylea HD is currently under consideration by the TGA. Treatment with 8mg Eylea HD may allow further extension of the treatment interval, potentially up to 12-16 weeks.
